An Overview Of Wisdom Teeth Removal Surgery & What To Expect
Wisdom teeth removal, also known as third molar extraction, is a common dental procedure performed to address potential complications associated with the growth and positioning of the third set of molars, commonly known as wisdom teeth. These teeth typically emerge in late adolescence or early adulthood, often leading to issues such as impaction, crowding, or improper alignment. As a result, many individuals undergo wisdom teeth removal surgery to alleviate pain, prevent dental problems, and safeguard overall oral health. The procedure is generally routine, but understanding the process, potential complications, and post-operative care is crucial for individuals preparing for this dental intervention. In this context, exploring the intricacies of wisdom teeth removal surgery becomes essential for those facing the prospect of undergoing this common dental procedure.
What are wisdom teeth, and why do they often require removal?
Wisdom teeth, also known as third molars, are the last set of molars located at the back of the mouth. These teeth typically emerge in late adolescence or early adulthood, usually between the ages of 17 and 25. While some people may not experience any issues with their wisdom teeth, many individuals face complications due to the size of their jaw and the late eruption of these molars.
Several reasons contribute to the common need for wisdom teeth removal:
- Impaction: Wisdom teeth often become impacted, meaning they don’t have enough space to properly emerge or grow in a normal position. This can lead to various problems, including pain, infection, and damage to adjacent teeth.
- Crowding: The jaw may not have enough space to accommodate the additional set of molars, leading to crowding. This can cause misalignment of existing teeth.
- Incorrect Angle: Wisdom teeth may emerge at an angle that can affect the alignment of neighboring teeth, leading to bite problems.
- Partial Eruption: Wisdom teeth may only partially emerge from the gums, creating a pocket where bacteria can accumulate, potentially causing infection and inflammation.
- Cysts and Tumors: In some cases, cysts or tumors may form around impacted wisdom teeth, causing damage to the jawbone and adjacent teeth.
- Pain and Discomfort: Even in the absence of specific complications, the eruption process itself can be painful and uncomfortable, leading individuals to seek removal for relief.
Due to these potential complications and the prevalence of issues associated with wisdom teeth, many dentists and oral surgeons recommend removal to prevent future problems and promote overall oral health. Regular dental check-ups and X-rays play a crucial role in monitoring the development of wisdom teeth and identifying potential issues early on.
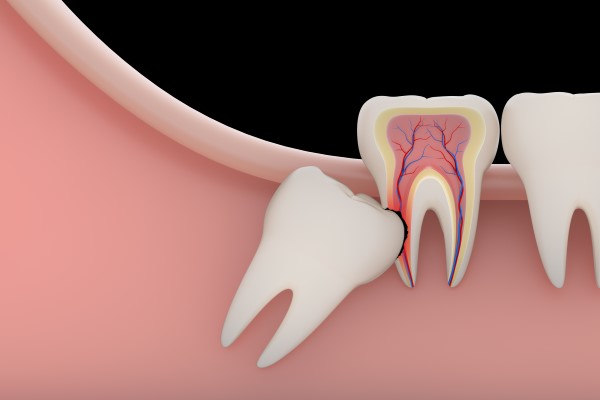
What are the common signs and symptoms that indicate a need for wisdom teeth removal?
The need for wisdom teeth removal is often signaled by various signs and symptoms. Persistent pain or discomfort in the back of the mouth, especially while chewing or biting down, can indicate issues with the eruption or positioning of wisdom teeth. Swelling, redness, and tenderness of the gums in the areas where the wisdom teeth are emerging may suggest inflammation or infection. Difficulty in opening the mouth fully, an unpleasant taste or odor, and persistent bad breath can also be indicative of problems with these molars. Additionally, recurring headaches and jaw pain may be associated with the misalignment or impaction of wisdom teeth, further highlighting the potential need for their removal. Regular dental check-ups, including X-rays to monitor the development of wisdom teeth, can help identify these symptoms early and guide appropriate intervention.
Wisdom Teeth Removal Procedure In 3 Steps
The Surgery Itself Takes 1 Hour To Complete
Preparation and Anesthesia
Before the actual procedure, the oral surgeon or dentist will assess the patient’s medical history, perform any necessary pre-operative examinations, and discuss the details of the surgery. On the day of the procedure, the patient is usually given anesthesia to ensure comfort and minimize pain during the surgery. The type of anesthesia can vary, with options ranging from local anesthesia to general anesthesia depending on the complexity of the extraction and the patient’s preference.
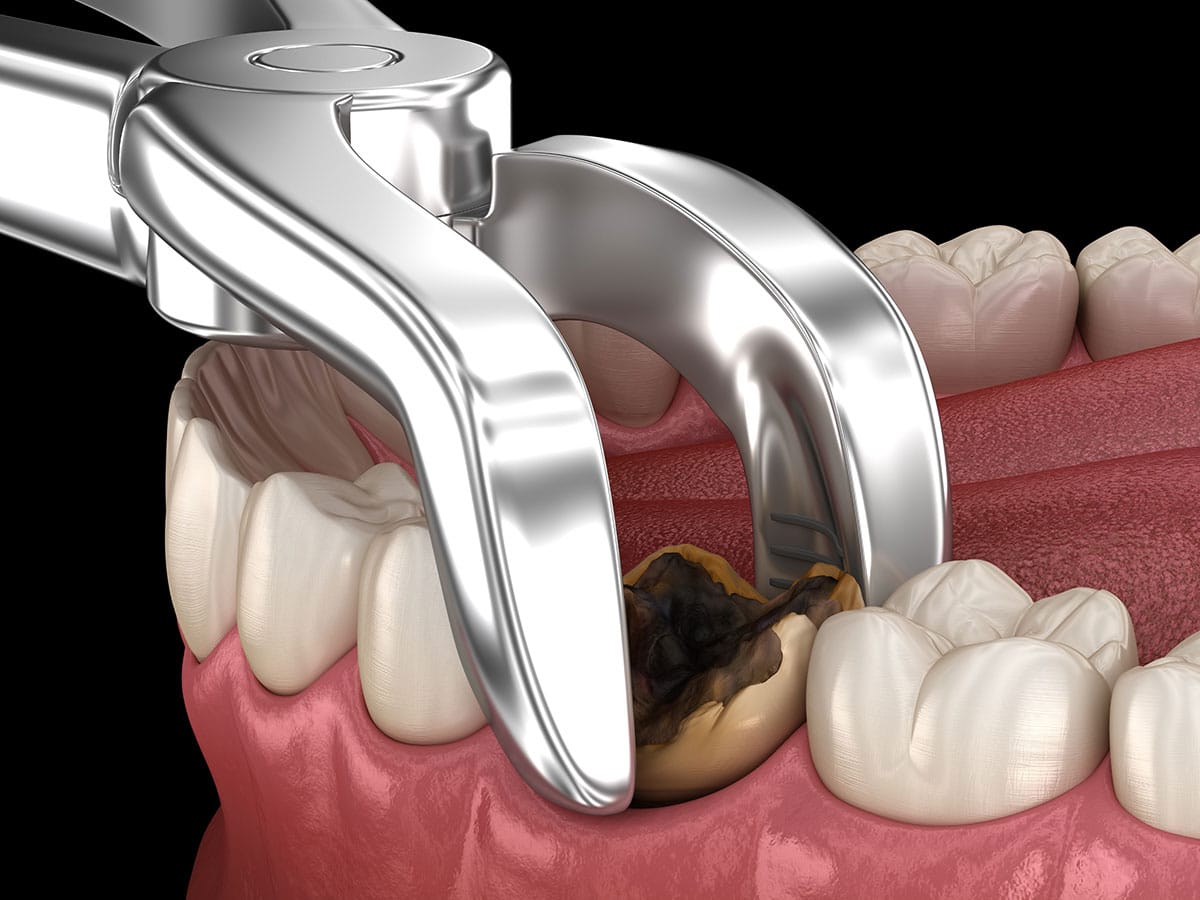
Extraction of Wisdom Teeth
Once the patient is properly anesthetized, the oral surgeon or dentist will proceed with the extraction. If the wisdom teeth are impacted, an incision may be made in the gums to access the teeth. In some cases, the teeth may need to be sectioned into smaller pieces for easier removal. The dentist or oral surgeon will carefully extract the wisdom teeth, taking care to minimize trauma to the surrounding tissues. The extraction site may be stitched up if necessary.
Post-Operative Care and Recovery Instructions
After the extraction, the patient will be monitored as they begin to wake from the anesthesia. Post-operative care instructions, including guidelines for managing swelling, pain, and bleeding, will be provided. Patients are usually advised to follow a soft diet for a few days, avoid certain activities that could disrupt the healing process, and adhere to prescribed medications or pain relievers as needed. Follow-up appointments are scheduled to monitor the healing progress and address any concerns.
Can wisdom teeth removal be performed under local anesthesia, or is general anesthesia commonly used?
Wisdom teeth removal can be performed under local anesthesia, and this is a common and routine approach for many cases. Local anesthesia involves numbing the specific area around the wisdom teeth, and the patient remains conscious during the procedure. While the patient may feel pressure and some movement, they should not experience pain.
General anesthesia is another option that can be used for wisdom teeth removal. This type of anesthesia induces a state of unconsciousness, and the patient is not aware of the procedure. General anesthesia is often chosen for more complex cases, multiple extractions, or for patients who may experience high levels of anxiety during dental procedures.
The decision between local and general anesthesia depends on various factors, including the complexity of the extraction, the patient’s medical history, and individual preferences. Dentists and oral surgeons will discuss these options with the patient before the procedure and make a recommendation based on the specific circumstances. Both local and general anesthesia are generally safe when administered by trained and qualified dental professionals.

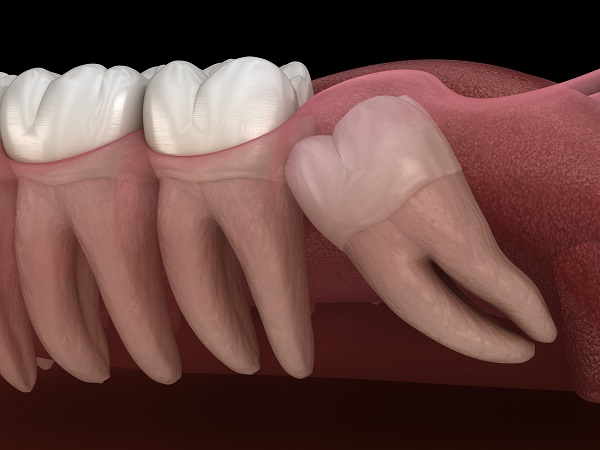
Are there different types of impaction, and how does the type of impaction influence the removal procedure?
Yes, there are different types of impaction when it comes to wisdom teeth, and the type of impaction can influence the removal procedure. The various types of impaction are classified based on the position of the wisdom teeth relative to the jawbone and surrounding teeth. The common types of impaction include:
- Soft Tissue Impaction:
- The wisdom tooth has partially erupted through the gum tissue but is still covered by a flap of gum.
- This type can be more susceptible to infection due to the challenge of keeping the area clean.
- Partial Bony Impaction:
- The wisdom tooth has partially erupted, but some of it remains trapped within the jawbone.
- This type may require more complex extraction techniques.
- Complete Bony Impaction:
- The wisdom tooth is fully encased in the jawbone and has not erupted through the gum.
- Complete bony impaction often requires more involved surgical procedures, such as sectioning the tooth into smaller pieces for removal.
The type of impaction influences the removal procedure because it determines the level of difficulty and complexity involved. For example:
- Soft tissue impactions: These may require a relatively simpler extraction procedure, often involving the removal of gum tissue covering the tooth.
- Partial bony impactions: Extraction may involve both elevation of the gum tissue and removal of a portion of the jawbone to access and remove the tooth.
- Complete bony impactions: These typically involve more complex surgical techniques, including sectioning the tooth into smaller pieces for easier removal.
The decision on the approach to wisdom tooth removal depends on the type and degree of impaction, and it is typically made by the oral surgeon or dentist based on careful examination and diagnostic imaging. The goal is to safely and effectively remove the impacted wisdom tooth while minimizing potential complications and promoting optimal healing.
How long does it take for the surgical sites to heal, and what are the signs of a normal healing process?
The healing time for surgical sites after wisdom teeth removal can vary from person to person, but generally, significant initial healing occurs in the first one to two weeks. During this period, patients may experience some swelling, bruising, and mild discomfort. The formation of a blood clot at the extraction site is crucial for proper healing and should not be disturbed. As the days progress, the swelling tends to subside, and any initial discomfort can be managed with prescribed or over-the-counter pain medications. Complete healing, including the closure of the gum tissue and bone remodeling, may take several weeks to months. Signs of a normal healing process include a reduction in swelling and pain, the absence of persistent bleeding, and the gradual return to normal oral function. It’s essential for patients to follow post-operative care instructions, including maintaining good oral hygiene, attending follow-up appointments, and contacting their oral surgeon or dentist if they notice any signs of infection or other complications during the healing period.